Spontaneous Retropharyngeal Haematoma following anticoagulant therapy: A rare presentation
P Adhikari, B Sinha, D Baskota
Citation
P Adhikari, B Sinha, D Baskota. Spontaneous Retropharyngeal Haematoma following anticoagulant therapy: A rare presentation. The Internet Journal of Head and Neck Surgery. 2008 Volume 3 Number 1.
Abstract
Anticoagulant therapy is routinely prescribed for the primary prevention of embolic events. It can lead to bleeding from different sites, so we should be cautious of this complication and patients with anticoagulant therapy should be monitored by coagulation tests. Here, we report a case of retropharyngeal haematoma developed spontaneously after anticoagulant therapy.
Introduction
Bleeding, internal or external, remains the major complication with anticoagulant therapy. Retropharyngeal haematoma, although extremely uncommon is a well known complication of cervical trauma, surgery, retropharyngeal sepsis, carotid aneurysm and internal jugular vein rupture.1 It has been reported to occur spontaneously in patients with bleeding disorders. Management is mainly supportive.
Case Report
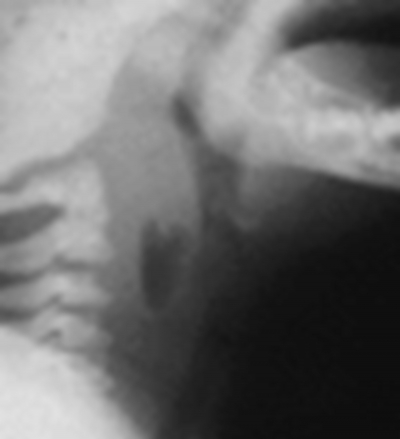
A 56 years old female, a diagnosed case of thrombotic micro-angiopathy on warfarin therapy, presented to Department of ENT and Head and Neck Surgery, TU Teaching Hospital with complain of dysphagia, shortness of breath and odynophagia for 3 days duration. Examination revealed a huge buldge in posterior pharyngeal wall along with neck tenderness. Patient was ill looking and on distress with tachypnea and tachycardia. Coagulation profile was done and International Normalized Ratio (INR) was 5.8. X-ray soft tissue neck lateral view revealed widening of prevertebral space with gas shadow (Fig:1).
Figure 1
She was managed conservatively with vitamin K and fresh frozen plasma. She became completely well in 8 days and discharged from hospital.
Discussion
Bleeding is the most common complication with oral anticoagulation. Hemorrhagic complications from warfarin treatment accounts for 10.5% of all adverse drug reactions resulting in hospital admission.2 Retropharyngeal haematomas are uncommon but are a recognized complication of cervical spine trauma, great vessel trauma, foreign body ingestion, violent coughing or sneezing, retropharyngeal infections and iatrogenic injury after procedures such as internal jugular line insertion.3 Eighteen cases of retropharyngeal haematoma secondary to oral anticoagulation have been reported previously.4
Patients classically present with Capp’s triad which includes compression of trachea and oesophagus, displacement of trachea anteriorly and bruising of the neck and chest.5 The initial symptoms of airway compression may include dyspnea, dysphagia, stridor, odynophagia, hoarseness and neck pain.6 The diagnosis is aided by a lateral x-ray of the neck which shows a widening of the prevertebral space.1 Computerized tomography scan is a better investigation to confirm the diagnosis and to assess the extent of the haematoma and its reaction to the neck structures.6
Although treatment course may vary depending on the aetiology of the haematoma, the first step in management is establishing definitive airway control.7 Patients with small, non-expanding haematomas can be treated conservatively with cervical spine immobilizatiobn and intravenous steroids.6 In high retropharyngeal haematoma producing significant airway obstruction, tracheostomy may be required.6
Correction of INR is essential as it prevents further bleeding. Vitamin K fresh frozen plasma or prothrombin complex concentrates are given. There is a little consensus in the literature regarding the use of steroids or prophylactic antibiotics in patients with retropharyngeal haematoma.3 Surgical drainage is essential for large haematomas and in rapidly expanding haemotomas.6
Conclusion
Retropharyngeal haematoma is an uncommon but potential life threatening condition if it progress to airway obstruction. Correction of INR with vitamin K and prothrombin complex concentrates is essential.
Correspondence to
Dr. Prakash Adhikari, MBBS, MS Resident., Department of ENT and Head and Neck Surgery, Ganesh Man Singh Memorial Academy of ENT and Head and Neck Studies, TU Teaching Hospital, Kathmandu, Nepal. Email: prakash_ooz@hotmail.com.