Anal Cancer In Pregnancy
S Wijesiri, O Orimogunje, V Bamigboye, M Kausha
Citation
S Wijesiri, O Orimogunje, V Bamigboye, M Kausha. Anal Cancer In Pregnancy. The Internet Journal of Gynecology and Obstetrics. 2010 Volume 15 Number 2.
Abstract
According to Cancer Research UK, anal cancer is a rare cancer; around 930 people are diagnosed in the United Kingdom each year. It is slightly more common in women than men, with rates increasing in women over the past 10 years. Around 8 out of 10 (80%) people diagnosed with anal cancer have evidence of Human Papillomavirus (HPV) infection in the anal area. Of the different types of HPV, type 16 is the most common in anal cancer. Invasive anal cancer is thought to develop from the growth of abnormal cells (squamous intraepithelial lesions) caused by HPV infection (1). Eighty-five percent of the anal cancers occur in the anal canal and 15% in the anal margin. There have been reported increased incidences of infection with HPV associated with female gender, with identified risk factors such as lifetime number of sexual partners, genital warts, receptive anal intercourse, and infection with human immunodeficiency virus (HIV) (2).
Introduction
Genital wart is associated with HPV, and its incidence has been increasing in recent years. This may explain, at least partly, the increasing incidence of anal cancer especially in younger women. Disease in women is primarily spread through vaginal intercourse. Anal condylomata can occur by extension from vulvar or perineal infection or by receptive anal intercourse. The risk of disease increases with the number of sexual partners (2).
In addition to the aetiological association with condyloma acuminatum, HPV infection is also associated with anogenital squamous intraepithelial lesions and other malignancy in the genital tract (cervical, vaginal, vulval, penile, anal); and head and neck lesions.
Most pregnant women infected with HPV and have had genital warts in the past usually have healthy pregnancies and smooth birthing experiences. The occurrence of genital warts while pregnant can be a foremost basis of apprehension for mothers to be. It puts the unborn child at risk of getting the infection. There is also a chance that genital warts can be passed along to newborn babies through a contaminated birth canal. However, significant size of genital warts during late stage of pregnancy not only increases risks of transmitting to the baby, it also poses significant obstetric difficulties.
Case Study
A 28 old gravida 3 para 2 at 33 weeks of gestation was admitted to the emergency department with painless bleeding from large genital warts.
Past medical and gynecological history revealed asthma and an 8 year history of genital warts, which have been treated with diathermy/cauterization. Furthermore, she had an abnormal smear test, which had not been investigated further. Obstetric history showed that the patient had two previous spontaneous vaginal deliveries in the previous 5 years.
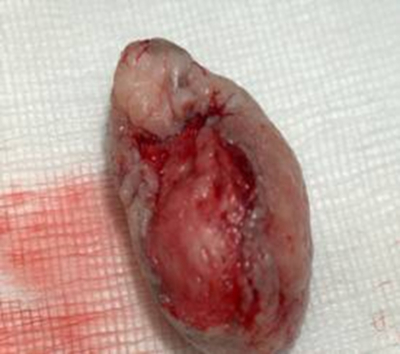
On examination; a 5-6 cm lesion was noted on the 6 o’clock position in the anal verge (Figure1), which was bleeding, and over the next 72 hours the patient lost significant amount of blood. With the ongoing bleeding, a decision was made to deliver the baby by caesarean section and simultaneously excise the anal lesion by a multi disciplinary team of obstetricians, paediatricians and general surgeons. At caesarean section, a 2.5kg male infant was delivered with good apgar scores and cared for in the special care baby unit. Following caesarian section, patient had her anal lesion excised by surgeons (Figure3-4). Post operatively, an MRI scan of pelvis was performed to assess the extension of the lesion and to stage the disease (Figure2).
The excised lesion on histopathology diagnosis confirmed an invasive squamous cell carcinoma in the external anal sphincter / canal (Figure5/ 6).
Outcome
Following histopathological diagnosis, the patient has been referred to specialist oncological treatment centre for further treatment.
Discussion
Bjørge et al (3) have shown prospective epidemiological evidence of an association between infection with HPV 16 and 18 and anal and perianal skin cancer. The delay in seeking treatment for genital warts, could have accounted for the subsequent malignant transformation in this young woman.
Creasman et al (4) have reported malignant transformation in 15 patients with “ordinary” condylomata acuminata. With pregnancy, the symptoms of genital warts get worse; mainly due to physiological suppression of the immune system, making the woman more susceptible to infections and viruses. Thus, genital warts may become larger in pregnancy. This leads to numerous complications when managing the pregnancy and delivery.
This patient having her immunity temporarily compromised with repeated pregnancies over the last 8 years of her life and inadequate treatment for Condyloma Acuminatum could account for the progression of this patient’s lesion to an invasive squamous cell carcinoma. Therefore young women should be advised to have treatment for genital warts to avoid this risk of malignant transformation, which can have significant impact on their lives.
Learning Objective
-
Education, adequate treatment and follow up are needed for patients diagnosed with genital warts prior, during and post pregnancy.
-
Pre conception counseling for the patients diagnosed with genital warts and/or HPV infections.
Acknowledgment
With special thanks to Dr M Witkowski (Consultant Histopathologist) & Ms. Joanne Shawcross (Academic Liaison Librarian- Furness General Hospital) .