Fetal Intracranial Tumor – A Case Report
A Ferreira, A Franco, A Paramos, A Silva, O Viseu
Keywords
fetal intracranial tumor, prenatal diagnosis
Citation
A Ferreira, A Franco, A Paramos, A Silva, O Viseu. Fetal Intracranial Tumor – A Case Report. The Internet Journal of Gynecology and Obstetrics. 2009 Volume 14 Number 1.
Abstract
The fetal intracranial tumors are rare and his prognosis is poor. With routine use of antenatal ultrasound screening, a large number of such tumors have been diagnosed.The authors describe a clinical case of a fetal intracranial tumor with prenatal diagnosis to 25 weeks of gestation, in Faro Hospital. Ultrasound examination showed a large solid intracranial fetal tumor. The MRI confirmed the diagnosis and showed hydrocephalus, macrocephaly and polyhydramnios.At 33 weeks pregnancy was interrupted by premature rupture of membranes, by caesarean section. Due to the size of the tumor and the extensive involvement brain could not establish any type of therapy. The newborn died after 10 minute of life. The primitive brain tumors are rare, rapid growth and have a poor prognosis.
Introduction
Fetal intracranial tumors are rare and usually fatal 1,2,3,7. Only 5% of childhood brain tumors arise in fetal live and their prognosis is poor.2 The diagnosis is usually made by ultrasonography in fetal life, as diagnosis of an intracranial mass, disrupting normal architecture with or without hydrocephalus 2,4,7 . Teratoma is the most common tumor in neonatal period making up one-half to one-third of tumors 1,2,3,5,7 .
Magnetic Resonance (MR) imaging can be used to improve imaging of fetal brain structures or abnormalities 2 .
We report a case of fetal intracranial teratoma diagnosed at 25 weeks of gestation after prior normal sonographic examinations.
Case Report
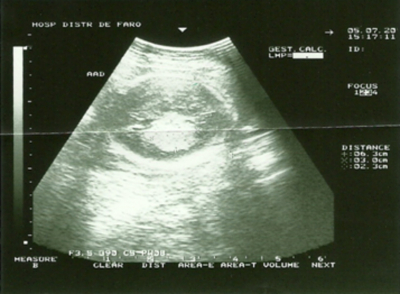
A 28-year-old woman, gravida 4 para 2 (a normal vaginal delivery at 33 weeks with premature rupture of the membranes and 2 miscarriages) had her antenatal surveillance in her family doctor. Ultrasonografic detailed examination was normal at 22 weeks. At 25 weeks of gestation, a 30x 23 mm heterogeneous intracranial fetal tumor was identified on ultrasound made in emergency (Figure.1) and she was referred for further management. The course of her pregnancy till then had been uneventful.
Figure 1
At 28 weeks the fetal magnetic resonance imaging showed an 80 mm heterogeneous mass with multiple cystic components involving left supratentorial regions and massively dilated lateral ventricles and this mass was causing hydrocephalus. No normal brain structures were identifiable (Figure 2).
Figure 2
The parents were extensively informed of poor prognosis for the baby but they decided not to terminate the pregnancy. The asked for another opinion in another hospital and at 32 weeks made another magnetic resonance imaging that showed a large increase of the tumor mass, severe obstructive hydrocephalus, no normal brain architecture were identifiable. Polyhydramnios, macrocephaly were founded (Figure 3).
Figure 3
At 33 weeks `gestation preterm labor started spontaneously by premature rupture of the membranes and a 3890 gr male fetus was delivered by cesarean section due to large fetal cranium with an apgar score of 1/4. Due to the size of the tumor and the extensive involvement brain could not establish any type of therapy. The newborn died 10 minutes after delivery.
A postmortem examination found a severely hydrocephalic brain and a large 8 cm intracerebral tumor replacing the entire left cerebral hemisphere. Histological examination showed an immature teratoma.
Discussion
Central nervous system tumors occur considerably less often in fetus and neonates that in older children. Their location, biologic behavior, response to therapy and histologic types are different. Only 5 % of childhood brain tumors arise in fetal and their prognosis is poor 2.
Teratomas are the most common congenital tumors 1,3,4,5,6. However, in only 2% of all cases the tumor is located intracranially and arises from central nervous system 5 . Congenital teratomas are most commonly found in sacrococcygeal region, but they also occur in the neck, mediastinum, and - as in our case – within the intracranial region, where the malignancy may arise 1. Teratoma is composed of tissues originating from all three germinal layers, and may occur in a variety of locations 4. Most are located in the pineal region, but about 20% are located in the suprasellar or infrasellar regions. In contrast to the infratentorial location in older children, most congenital intracranial tumors are of supratentorial origin 3. Histologically they are classified as mature, immature or teratoma with malignant components based on the amount of tissue differentiation 2.
With routine use of antenatal ultrasound imaging a larger number of such tumors have been diagnosed 2,5. Intracranial teratomas appear as irregular echogenic masses with transonic areas 5.
Cystic tumors and teratomas are usually characterized by completed loss of normal intracranial architecture. The most common initial ultrasonographic finding in fetus is macrocephaly, and additional features typically include gross distortion or replacement of normal brain tissue by echogenic mass with multiple cystic components, as well as hydrocephalus secondary to obstruction 4.
The differential diagnosis includes other intracranial neoplasms, hydrocephalus, hydrancephaly, holoprosencephaly, porencephaly, arachnoids cysts and meningo-encephaloceles 4,5.
Several recent case reports have described the use of magnetic resonance imaging between 25 and 36 weeks in helping confirm the diagnosis of intracranial teratoma 4.
Polyhydramnios is also frequently associated with intracranial tumors 3.
Obstetric management is dependent on gestational age at the time of diagnosis. If the tumor is detected early in pregnancy, the parents should consider terminating the pregnancy. These tumors may grow to excessive proportion and most of them are first diagnosed at an advanced gestational age 3. Another important factor is the type of delivery. Fetuses with hydrocephalus of brain tumors have increased intracranial pressure (ICP). The pressure exerted by mother´s abdominal wall during the uterine contractions at delivery is transmitted to the intracranial cavity of the fetus, considerably raising the ICP, which may influence the prognosis. Cesarean section should be performed before the labor stars 2. The incidence of cesarean section is still 60.4%, because cephalopelvic disproportion is common 3. The optimal mode of delivery is controversial and the choice made needs to balance the maternal risk of cesarean section against the possibility of cephalopelvic disproportion and successful induction of labour in a preterm gestation 6.
Although technological improvements have made the diagnosis easier, the same situation was not valid for the treatment. There are still few therapeutic options and a poor outcome is usually unavoidable 2.
In spite of recent advances in neonatal surgery and the availability of additional therapeutic strategies, all cases with fetal intracranial tumors still have a very poor prognosis 3.