Folliculotropic Mycosis Fungoides
K Rojas, R Talpur, C Torres-Cabala, M Duvic
Keywords
cutaneous t-cell lymphoma, mycosis fungoides
Citation
K Rojas, R Talpur, C Torres-Cabala, M Duvic. Folliculotropic Mycosis Fungoides. The Internet Journal of Dermatology. 2009 Volume 8 Number 1.
Abstract
Folliculotropic mycosis fungoides (FMF) is a variant of mycosis fungoides characterized by the presence of folliculotropic infiltrates, often with sparing of the epidermis, and preferential involvement of the head and neck. We report a case with classical FMF lesions but also with a deep ulcer, which is an unusual presentation.
Abbreviations: MF- Mycosis Fungoides,
Introduction
Folliculotropic mycosis fungoides has been designated as a distinct entity in the World Health Organization-European Organization for Research and Treatment of Cancer classification system for cutaneous lymphomas. 1 It usually involves the scalp and face but may also compromise the torso, as in our patient. Its clinical spectrum includes scarring and nonscarring alopecias, erythematous plaques with follicular accentuation, acneiform lesions such as nodulocystic lesions, pustules, milia and comedones; tumors and sometimes mucinous discharge. Severe pruritus is also a prominent feature.2
Case Report
A 62-year-old man presented with a 20 year history of a pruritic erythematous rash on his scalp and trunk previously diagnosed as seborrheic dermatitis and eosinophilic folliculitis. He had eosinophilia (13%) and IgE significantly elevated (2317 K/UL). He was initially treated with antifungals, topical steroids, antihistaminics and oral antibiotics with partial improvement. This past last year, he developed a slowly growing ulceration in the middle of his back.
Physical examination revealed (Figure 1A) an erythematous plaque with scarring alopecia on his scalp and (Figure 1B) erythematous telangiectatic patches and plaques on the trunk. Micropustules were seen within some of these lesions. (Figure 1C). On the back, he had a large 4x3 cm. ulcer down to the muscle containing purulent drainage (Figure 1D) and had palpable axillary and inguinal nodes. The cultures grew
Diagnosis: The patient was diagnosed with Folliculotropic mycosis fungoides stage IIA (T2N0M0).
Microscopic findings and clinical course
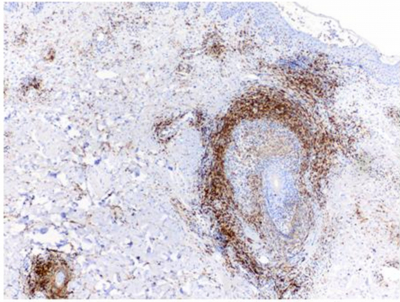
Two sets of biopsies were examined. The initial biopsy (dated 2002) showed a mild perifollicular infiltrate composed of lymphocytes and some eosinophils. A few eosinophils were reported to be present in the epidermis. A diagnosis of eosinophilic folliculitis was made in an outside institution. Subsequent in house biopsies, taken 6 years later, showed a dense lymphocytic infiltrate with prominent folliculotropism. Some epidermotropic cells were also seen. (Figure 2A) The infiltrating lymphocytes displayed mild cytologic atypia (Figure 2B). Plasma cells and eosinophils were also present. Immunohistochemical studies revealed the lymphocytes to be CD3-positive T cells (Figure 2C); rare CD20-positive B cells were identified. The folliculotropic and epidermotropic lymphocytes were mainly CD4 positive (Figure 2D). Scattered CD8-positive cells were seen within the follicles and epidermis (Figure 2E). Diffuse (greater than 75%) positivity for CD25 by the atypical lymphocytes was observed in one of the biopsies. Re-examination of the original biopsy showed a population of atypical, epidermotropic CD3-positive lymphocytes, positive for CD4 and negative for CD8. The epidermotropic and folliculotropic lymphocytes show a CD4:CD8 ratio of about 4:1. A diagnosis of mycosis fungoides, folliculotropic, was made on both sets of specimens. Molecular studies for TCR gamma gene rearrangement identified a monoclonal population, supporting the diagnosis of mycosis fungoides.
Lymph node biopsy showed follicular hyperplasia.
The clinical course was consistent with folliculotropic mycosis fungoides IIA. He was initiated on bexarotene 150 mg and dicloxacillin 500 mg daily with considerable improvement of cutaneous lesions (Figure 3A, B, C and D). Patient developed new papules on lower extremity and was started on nitrogen mustard alternating with betamethasone.
Discussion
Five distinctive histological patterns have been described in FMF, which are considered to be highly characteristic. They include prototypical changes with intact follicles with folliculotropism with or without mucin, basalloid folliculolymphoid hyperplasia, cystic, granulomatous and eosinophilic folliculitis subtypes. Our patient not only presented with classical FMF lesions but also with a deep ulcer, which is an unusual presentation.
The eosinophilic folliculitis pattern as in our patient, can be prominent and might be associated to misdiagnosis, but should be considered to establish FMF. 3 Hypereosinophilia and elevated Ig E levels have been reported in mycosis fungoides in the absence of any other underlying cause4 but not in FMF. In advanced stages of CTCL, a shift in cytokine profile from TH1 to TH2 is observed, which coincides with eosinophilia, high levels of immunoglobulin E, and increased susceptibility to bacterial infections.5 These features might be associated with long course FMF but not necessarily with advanced stages.
FMF has an aggressive path; it is more refractory to treatment and has a worse prognosis than the classic type of MF. Best results have been reported with psoralen plus UVA (PUVA) therapy with oral bexarotene or PUVA with interferon alfa.2,6 However, it has been reported complete response with low dose (150mg) oral bexarotene monotherapy in a patient with acneiform lesions on her face and back, similar to our patient.7
FMF may present with atypical clinical and histological features, therefore it’s diagnostic and treatment might be delayed.