Acute Cholecystitis In A Child With HAV Infection
A Venuta, P Bertolani
Keywords
cholecystitis, hepatitis, hepatitis-a-virus hav
Citation
A Venuta, P Bertolani. Acute Cholecystitis In A Child With HAV Infection. The Internet Journal of Pediatrics and Neonatology. 2006 Volume 6 Number 2.
Abstract
We report a case of acute cholecystitis in a 2-year-old male child with hepatitis A virus (HAV) infection. The occurrence of this complication is rare, but must be kept in mind, as it can lead to gangrene and perforation of cholecystic wall and become a surgical emergency
Case Report
A 2 year-old male child of Iranian ancestry, but living in Italy, was admitted with jaundice following four days of relapsing-remitting high fever, nausea and vomiting. On the third day he presented with a febrile generalised convulsion. On examination he appeared jaundiced and dehydrated. His temperature was 39°C, the respiratory rate was 40/min and he was tachycardic (110/min). The right upper quadrant of his abdomen was tender with an exquisite Murphy sign. Mild splenomegaly was also observed. There were no features of meningism and no signs of neurodeficit.
Laboratory studies found a haematocrit of 28%, a low WBC count (3.500/mm3), elevated C reactive protein (12.5 mg/dL), elevated AST (1020 U/L) and ALT (550 U/L), increased total bilirubinemia (5.8 mg/dL) with a direct fraction of 2.8 mg/dL, and prothrombin activity 63%. Serology for viral hepatitis suggested acute hepatitis A infection (anti HAV IgM +), and was negative for other causes (HBsAg (-), anti HBcIgM (-), anti HCV (-)). Serology for salmonellosis and brucellosis were negative. Three serial blood cultures were negative. Stool culture and parasitological examination were negative.
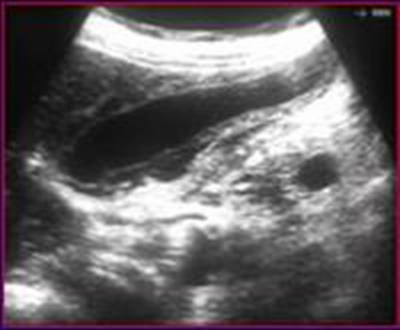
An abdominal ultrasound showed hepatomegaly and increased volume of the gallbladder with no gallstones. Its wall was markedly thickened and microabscesses were noted. A small amount of pericholecystic fluid was present. Sonographic Murphy sign was elicited when the probe was pushed directely on the gallblabber. (Figure1.)
Figure 1
The child was transferred to a surgical ward under observation for conservative treatment. In the following five days symptoms and signs slowly regressed. An abdominal ultrasound was repeated at discharge, 10 days after admission: the gallbladder wall appeared normal and the pericholecystic fluid was reabsorbed. AST was 110 U/L and ALT 249 U/L, WBC count was 5.900 mm3 and thrombocytosis was present (690.000 mm3). At 3-month follow up he was doing well.
Discussion
Our infant had clinical and echographic signs of cholecystitis during an episode of hepatitis A. Acute cholecystitis in the course of HAV infection is a rare event. Only few cases have been described in adults 1 , 2 , 3 . Mourani et al. reported a case of a 68-year-old man who underwent surgery; an immunohistochemical analysis demonstrated that HAV infected the epithelium of both the intrahepatic bile ducts and the gallbladder 2 . These findings demonstrate that HAV can play a direct role in the pathogenesis of cholestasis and gallbladder abnormalities in course of HAV hepatitis.
Black et al. 4 described a 6-year-old boy admitted to hospital with acute gangrenous cholecystitis requiring emergency cholecystectomy. Examination of the gall-bladder revealed severe inflammation with areas of haemorrhage and necrosis and mucosal sloughing; serology confirmed hepatitis A infection.
Casha et al. 5 reported a 12-year-old girl with abdominal pain and fever with clinical features of cholecystitis. Echography showed thickening of gallbladder wall. In the following days jaundice appeared and HAV hepatitis was demonstrated.
We therefore conclude that cholecystitis is a rare complication of HAV infection that must be kept in mind, as it can lead to gangrene and perforation of cholecystic wall and become a surgical emergency.