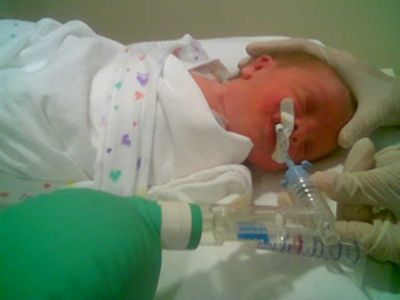
Orotracheal Continuous Positive Airway Pressure With a Compensation Bag: A Preliminary Report About a New Technique for Assisted Ventilation in Premature Infants
G Alberto Orozco, V Rosa María Estrada
Keywords
compensation bag, neonatal respiratory failure, orotracheal continuous positive airway pressure cpap, respiratory physiology
Citation
G Alberto Orozco, V Rosa María Estrada. Orotracheal Continuous Positive Airway Pressure With a Compensation Bag: A Preliminary Report About a New Technique for Assisted Ventilation in Premature Infants. The Internet Journal of Pediatrics and Neonatology. 2008 Volume 10 Number 2.
Abstract
Objective: We used a rubber bag adapted for ventilation with orotracheal continuous positive airway pressure (CPAP), to provide constant alveolar distention pressure and alveolar stability while compensating for pressure or volume changes from physiological events like coughing or crying. Materials and Methods: We administered orotracheal CPAP with compensation bag to nine newborns with mean weight of 1077 g (range, 779-1311 g) and mean gestational age of 28.5 weeks (range, 26 - 30 weeks). All infants underwent measurement of blood gases and vital signs, and chest radiographs.
Introduction
Advances in the intensive care of the newborn are closely related to evolution in the management of respiratory distress syndrome. Respiratory distress syndrome is frequently associated with lung immaturity, especially in premature infants, and with various pathological conditions in the mature lung of the full-term baby. The best ventilatory technique is one that stabilizes pO2, pCO2, and pH, avoids trauma due to volume and pressure, reduces the possibility of pulmonary injury, and shortens the time spent in the hospital. The modalities of ventilatory assistance range from the more benign continuous positive airway pressure (CPAP) to conventional mechanical ventilation and high frequency ventilation. However, the principal objective in selecting the mode of respiratory support should be to minimize trauma due to volume and pressure.
In the past three decades, the objectives in treating respiratory problems in premature infants have changed, becoming more ambitious. In the 1970s, the main objective was to lower mortality rates; in the 1980s, to avoid or minimize neurological damage; in the 1990s, to diminish pulmonary injury; and since 2000, the aims have been to shorten the length of hospital stay and minimize pulmonary damage.
CPAP has been used to treat respiratory distress syndrome since 1973 (1); after 1980 intermittent mandatory ventilation replaced this form of ventilation as the most popular ventilation worldwide, but since 1987, nasal CPAP has become more common because it is easy, safe, less expensive, and carries a lower risk of bronchopulmonary dysplasia (3)(7)(13). Nasal CPAP reduces the need for synchronized mandatory ventilation, risk of pulmonary injury, and length of hospitalization (1)(2)(13). The need for mechanical ventilation increases with earlier prematurity and severe pulmonary pathology that causes increased respiratory problems, which in turn may augment the alveolar oxygen tension gradient and worsen pulmonary damage (7). Early nasal CPAP has become the initial management for these babies; however, some factors can limit its effectiveness and safety. Pressure changes due to physiological events such as crying, mouth opening or closing, coughing, or hiccupping can affect alveolar stability. In a large randomized trial, Morley and colleagues found significantly greater benefit in newborns treated with nasal CPAP with prongs compared with mechanical ventilation; however, barotrauma was more frequent with nasal CPAP (9%) compared with mechanical ventilation (3%) (13).
In the past, CPAP was administered via endotracheal cannula; however, this method of ventilation was abandoned due to the high risk of barotrauma caused by surges of pressure in a closed rigid system that eventually generated increased resistance and a risk of air leakage (8). This increased resistance was considered a significant risk and limited the use of orotracheal CPAP, particularly in premature infants.
The purpose of this report is to present a new physiological concept in ventilatory support, designed to improve the performance of CPAP and diminish the inherent risks of conventional mechanical ventilation or nasal and orotracheal CPAP in the management of acute respiratory failure in premature and low-weight infants.
The Concept of the Compensation Bag (Accessory Lung)
The compensation bag is based on the principle that pressure in a closed airway circuit always tries to find a way to escape. In mechanical ventilation, the weakest point in the closed circuit is the alveolus; therefore, any variation in pressure will be directly reflected in alveolar pressure. That is, if pressure in the circuit decreases, intra-alveolar pressure decreases, resulting in a decrease in the alveolar oxygen tension gradient and collapse of the alveolar sac. On the other hand, increased pressure in the airway circuit will increase intra-alveolar pressure, resulting in distention of the alveolar sacs, inflammatory changes in the alveolar wall, and eventual alveolar rupture and air leakage. In the long term, this gives rise to pathological sequelae such as bronchopulmonary dysplasia.
The compensation bag is fitted with a commercially available distensible mechanical bag that is interposed in the closed circuit; therefore, when pressure increases, distention will occur in the bag and not the alveolus (Figure 1, Figure 2).
Figure 1
Figure 2
The bag transforms the respiratory system of the baby into a high-volume system. When pressure increases, the bag expands and maintains optimal expansion of the alveoli without risk of overdistention. At the same time, pulmonary resistance is regulated within the circuit, improving ventilation through better alveolar expansion and oxygen tension. This mechanism prevents sudden pressure variations but maintains the benefit of conventional CPAP, keeping a constant alveolar volume regardless of physiological events.
Methods and Materials
We studied nine premature newborn infants with acute respiratory failure. Their gestational ages varied from 26 to 30 weeks (mean, 28.5 weeks), and they weighed between 779 and 1311 g (mean, 1077 g). All patients were orotracheally intubated and given the recommended dose of bovine surfactant (Survanta, Ross Products Division, Abbott Laboratories Inc, Abbot Park, Illinois, USA). Before intubation, we gave intermittent positive pressure for 10 minutes for alveolar recruitment. After intubation, the babies were ventilated with CPAP, using warm humidified oxygen and a commercially available interposing neonatal reanimation bag. The bag was a hyperinflation 0.5 L bag with a pressure-limiting elbow and a disposable manometer (SIMS Portex Inc. Keene NH 03431, ref. 008430vm).
Arterial gases, transcutaneous oxygen saturation, cardiac frequency and rhythm, and arterial pressure were constantly monitored. We performed chest radiographs daily to detect the presence of barotrauma or air leaks, and the pressure of the ventilatory system was kept constant at 5 mm Hg.
Results
Eight patients required only one type of ventilatory mode, CPAP, for effective treatment. One patient required high-frequency oscillatory ventilation on day 3 due to pulmonary arterial hypertension manifested by hypoxemia and reduced arterial blood pH Tracheal intubation was maintained for an average of 86 hours (range, 54-108 hours) in the eight patients in whom the treatment was successful. None of the eight infants showed evidence of air leakage, bronchopulmonary dysplasia, patent ductus arteriosus, intraventricular hemorrhage, or infection attributable to the procedure. In all patients, stable flow-volume curves were obtained (Figures 3 and 4), with symmetrical curves with no spiking or dipping in pressure.
Figure 3
Figure 4
The gasometric determinations were similar in all patients, including the patient who required high-frequency oscillatory ventilation. The gasometric data showed an initial period of hyperoxemia (Figure 5) and a rapid fall of pCO2 (Figure 6). The pH remained stable in all babies (Figure 7). We used permissive hypercapnia, and the highest pCO2 was 60 mm Hg (Figure 6). Figure 8 shows the gasometric data in the patient who required high-frequency oscillatory ventilation.
Figure 5
Figure 6
Figure 7
Conclusions
We conclude that CPAP implemented with a compensation bag obtained high pulmonary volume and alveolar stability in premature infants with acute respiratory failure. This technique provided controlled, stable, closed-circuit pressure that maintained elevated alveolar oxygen tension.
Constant pressure ventilation of 5 mm Hg is adequate for maintaining ventilatory support in newborns with low birth weight and acute respiratory failure. An inflating compensation bag is capable of absorbing increments in pressure, thus reducing the risk of air leakage and risk of lung injury by excessive volume or pressure. At the same time, the bag facilitates alveolar recruitment and permits the administration of positive end-expiratory pressure.
Further research is needed to confirm whether a compensation bag interposed in closed circuit ventilation is an improvement on currently available ventilatory techniques for the treatment of acute respiratory failure. In addition, further studies are needed as to the feasibility of using this method with nasal prongs.