CT findings in Gall stone induced Hemobilia: an unusual cause of massive GI bleed.
A Hakeem, H Shafi, T Gojwari, F Shaheen, R Rasool, S Rasool, A Bashir
Keywords
ct scan, gall stones, hemobilia
Citation
A Hakeem, H Shafi, T Gojwari, F Shaheen, R Rasool, S Rasool, A Bashir. CT findings in Gall stone induced Hemobilia: an unusual cause of massive GI bleed.. The Internet Journal of Gastroenterology. 2009 Volume 9 Number 1.
Abstract
Gallstone induced hemobilia is uncommon and can give rise to massive gastrointestinal bleed due to mucosal ulceration in a chronically thickened gall bladder wall. Strong clinical suspicion with in time endoscopy and CT Scan may be helpful in detecting the source of upper GI bleed and can guide for the surgical intervention to be done.
Case Report
A 65 years old female complained of biliary type of pain, vomiting, decreased appetite for one week. There was no history of fever, altered mentation, giddiness, abdominal distension, malena and hemetemesis. On physical examination patient was conscious oriented in time place and person with significant ictrus, pallor and pedal edema. Her pulse and blood pressure were 96 beats/minute and 130/70 mmHg respectively. Chest and cardiovascular examinations were clinically normal. Her abdominal examination showed swelling with tender right hypochondrium, positive Murphy’s sign with palpable gallbladder. Rest of the examination was unremarkable. Laboratory parameters were Hb. (12.0g/dl), WBC. (3.5-8.54), platelets. (103- 247), MCV(80-94.6),mchc (28.6),MCH (27.1),hct (41.9) ,urea 42, cr. 1.1, Na+ (138-147), K+ (3.08-4.2). The liver function tests were bil- (2.42-5.6),ast- (43-56),alt- (40-133),alp- (1038-1903),tp- (5.93-6.7),alb- (2.7-3.8). Her amylase was (543, 1389).Arterial blood gas, coaglugram and Chest x-ray were normal. On ultrasonograohy she had two calculi in gall bladder,one very big and 1 small calculus with echogenic material seen in gall bladder ? sludge. Common bile duct was dilated 1.2cm with stone at the lower end.
On the 3rd day of the hospital stay patient developed malena and dropped her blood pressure and hemoglobin to 6.4g/dl.there was persistent tachycardia. She was resuscitated with packed cells. The patient was endoscoped which showed normal esophagus, normal stomach full of blood, d1 -normal, d2 - fresh blood coming from papilla. ERCP was not done. After endoscopy an urgent CECT abdomen was planned. CT was done on Siemens spiral CT SCAN which showed hyperdense areas filling gall bladder with variable attenuation of +50 to +170 hounsfield value suggestive of calculi admixed with blood.
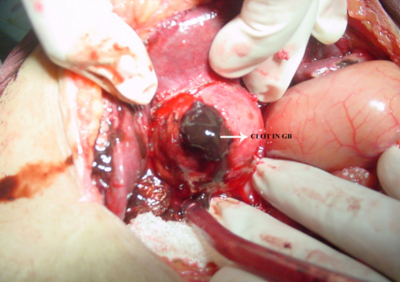
The hyperdense area extended upto terminal common bile duct having attenuation of +58 HU hence an impression of heamobilia was made. Emergency surgery was subsequently done.The intraoperative findings were; big epigastric hernia about 6x10cms. Gall bladder duodenum transverse colon and mesocolon matted together. Gall bladder full of fresh blood clots. One big and few small stones were found in gall bladder. Half of the mucosal wall ulcerated.
CBD opened and blood clots drained. However, clear bile was seen after normal saline wash. Cholecystectomy with CBD exploration with T tube drainage was done. Post operative period in hospital was uneventful. Biopsy report showed feature of chronic cholecystitis without any evidence of malignancy.
Discussion: The term hemobilia was first coined in 1948 by Sandblom(1) Hemobilia is basically an upper gastrointestinal bleed that originates from biliary tree. It was first reported by Francis Glisson in 1654 in a case of trauma right hypochondrium.(2).The first surgery to stop an upper gastrointestinal bleeding from biliary tree was done in 1895 in which total gastrectomy was done however patient could not survive more than 5 days(3). Kehr in 1903 did first successful operation for right hepatic artery aneurysm ruptured into gall bladder neck (4). First successful hepatic resection for hemobilia was done in 1957(5).A magnitude of diseases can result in hemobilia like trauma, cholelithiasis, acalculous inflammatory diseases, vascular disorders, and neoplasms etc.(6,7) Gallstone disease and cholecystitis constitute the rarest causes of hemobilia.(8).A high level of clinical suspicion of heamobilia has to be made if a gastrointestinal bleed develops with hypochondial tenderness and biliary type of pain and when other causes of gastrointestinal bleed have been excluded. A clinical suspicion should prompt confirmation of the diagnosis with angiography or endoscopy, but computed tomography or ultrasonography may also be helpful. CT scanning can show a distended gall bladder with contents of the gallbladder having attenuation of 67-82 HU, which is thought to be consistent with blood mixed with bile. In addition, some inhomogeneity of gallbladder contents, with denser regions in dependent portions measuring 81-91 HU can be also present, most likely representing clots.(9)
Careful consideration of the specific anatomy will help define the therapeutic options-angiography versus surgical intervention. The intervention depends on the severity of the hemorrhage and the extent of injury. The treatment of massive or persistent hemobilia is surgical drainage of hematoma and ligation of bleeding sites. Non-massive hemobilia may be treated conservatively with liver healing documented by serial selective arteriograms (10).